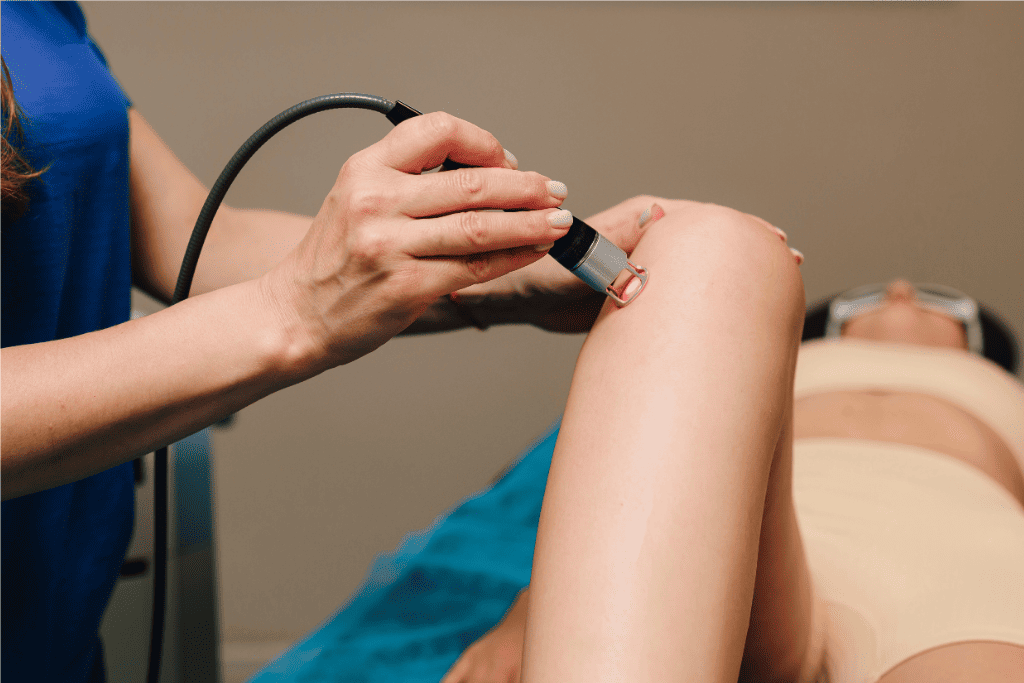
Can Cold Laser Therapy Help Delay or Prevent Surgery?
Exploring Alternatives Before Surgery
When joint or muscle pain persists for weeks or months, it can start to impact sleep, work, and daily activities. As the discomfort continues, many people worry that surgery might be the only option. This belief is common, especially when other treatments haven’t provided lasting relief.
However, orthopedic care usually starts with less invasive treatments. Doctors often try these first to see if the symptoms improve. The goal is to reduce inflammation, soothe irritated tissue, and help you move more easily.
One treatment that’s become more popular recently is low-level laser therapy, also known as cold laser therapy. It uses light energy to promote the healing of injured tissue.
People interested in laser therapy for pain often ask if it can help them avoid surgery. The answer depends on the type of injury. Sometimes, cold laser therapy can ease pain and swelling enough to delay or even avoid surgery.
Knowing how this therapy works can help you make better treatment decisions.
What Is Cold Laser Therapy?
Cold laser therapy is a non-invasive treatment that uses low-intensity light to promote healing of injured tissue. It’s also called low-level laser therapy or regenerative laser therapy.
Unlike surgical lasers, this treatment doesn’t cut or heat the tissue. Instead, it sends gentle light through the skin to reach muscles, tendons, ligaments, and other soft tissues beneath the skin.
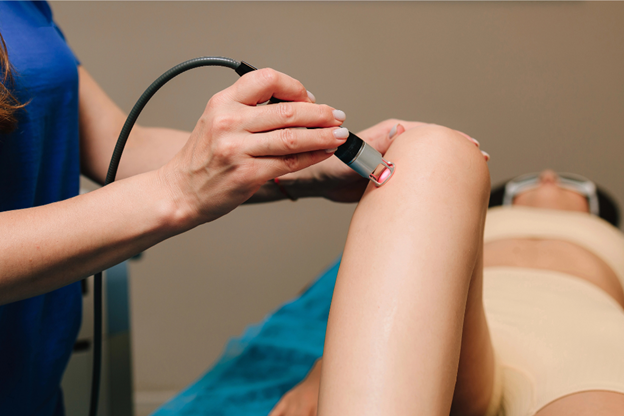
During a session, a clinician focuses the laser device on your skin over the painful spot. The device sends certain wavelengths of light that interact with the cells in that area.
The aim is to boost cellular activity and support your body’s natural healing. Most people feel little or nothing during the treatment.
Cold laser therapy is used to treat sports injuries, tendon problems, and ongoing joint pain.
How Cold Laser Therapy Works
Laser therapy for pain works by using light energy to interact with your body’s cells.
Laser light energy passes through the outer layers of the skin. The cells in the injured area absorb this energy and may respond in ways that help healing.
Researchers think several changes can happen in the body during laser treatment for inflammation.
- Cells may produce more energy, which helps them repair damaged tissue.
- Blood circulation may increase in the treated area.
- Oxygen and nutrients may reach injured tissue more easily.
- Inflammatory chemicals may decrease, thereby reducing swelling.
These changes can help reduce pain and make movement easier. As inflammation goes down, people often feel less stiff and move more freely.
Cold laser therapy tends to work best when used as part of a comprehensive treatment plan. Doctors often combine it with stretching, strengthening exercises, and other non-surgical treatments.
This approach supports healing and helps people safely return to their usual activities.
Orthopedic Conditions That May Benefit from Cold Laser Therapy
Cold laser therapy is often used for injuries involving soft-tissue irritation or inflammation. These conditions affect tendons, ligaments, muscles, and joints.
Doctors sometimes recommend cold laser therapy for:
- Tendonitis in the shoulder, knee, or elbow
- Ligament sprains from sports or physical activity
- Overuse injuries common in athletes
- Knee pain caused by tendon irritation
- Shoulder pain affecting tendons or bursae
- Tennis elbow and other elbow tendon injuries
- Muscle strains from sports or exercise
- Repetitive stress injuries related to work or activity
Some people also ask if cold laser therapy can help with herniated disc pain. While it doesn’t fix the disc, it may reduce inflammation around irritated nerves as well as in overlying muscles, helping ease pain for some.
Athletes and active adults often consider laser therapy to recover without a long break from their activities.
However, laser therapy works best when doctors know the exact cause of your pain.
Also Read: How Cold Laser Treatment Helps Speed Up Healing After Injury
Scenario: When Cold Laser Therapy May Help Delay Surgery
Imagine a patient who develops ongoing knee pain from running. The pain worsens over time and begins to affect daily activities.
An orthopedic evaluation shows tendon inflammation but no major structural damage. Because of this, the doctor recommends conservative care before considering surgery.
The treatment plan includes rest, strengthening exercises, and several sessions of low-level laser therapy.
Over a few weeks, swelling decreases and movement improves. The patient notices less pain when walking and gradually returns to light exercise.
This example highlights a common question: can cold laser therapy help delay surgery?
If inflammation improves and movement comes back, surgery might not be necessary. In other cases, feeling better may allow people to delay surgery for some time.
Still, results are different for everyone. Laser therapy can help with healing, but it can’t fix serious structural damage.
Benefits of Cold Laser Therapy for Orthopedic Patients
Patients in Los Angeles looking for non-surgical pain treatments often want options that are safe, convenient, and effective.
Cold laser therapy offers several advantages:
- It is non-invasive and does not require incisions.
- No anesthesia is needed during treatment.
- Sessions are usually short and done in an outpatient setting.
- Most patients return to normal activity right after treatment.
These advantages make cold laser therapy appealing to those seeking pain relief without the need for surgery.
Cold laser therapy also works well with other treatments. It can be combined with physical therapy, stretching, or changes in activity.
People looking for ways to avoid back surgery often try therapies like this as part of a conservative care plan.
It’s important to have realistic expectations. Laser therapy can help reduce inflammation and make you more comfortable, but it isn’t a cure for every orthopedic problem.
When Surgery May Still Be Necessary
Even though conservative treatments help many patients, surgery may still be required in some situations.
Severe structural damage often cannot heal without surgical repair. Examples include major ligament or tendon tears, unstable joints, or advanced cartilage loss.
Patients with severe joint degeneration may also need surgery when pain continues despite non-surgical care.
People who wonder if low-level laser therapy can prevent surgery often hope it works for every condition. In reality, the best treatment depends on the specific injury.
Laser therapy can help manage pain and inflammation, but it can’t rebuild severely damaged tissue.
In those situations, surgery may be the best long-term solution.
The Importance of an Accurate Orthopedic Diagnosis
Joint and muscle pain can have many causes. Two people with similar symptoms might actually have very different injuries.
An orthopedic evaluation can help find the exact cause of your pain.
Orthopedic specialists at Urgent Orthopaedic Care usually start with a physical exam to assess your range of motion, strength, and swelling. They may also use imaging tests like X-rays or MRI scans. These tests help doctors decide if cold laser therapy might be a good non-surgical option for you.
When treatment targets the actual cause of pain, you’re more likely to see positive results. Without a clear diagnosis, even advanced treatments might not be very effective.
What Patients Can Expect During Treatment
Cold laser therapy sessions are usually simple and quick.
You’ll sit or lie down comfortably while the clinician sets up the laser device or places a handheld laser device on your skin over the injured area. Which option is used depends on the body part as well as diagnosis being treated. You will be asked to wear protective eyewear during the session.
Most people feel little or nothing during the procedure. Some notice mild warmth or tingling, but discomfort is rare.
Doctors often recommend 2 sessions per week over a number of weeks depending on the chronicity of symptoms. This gives the therapy time to support healing.
Cold laser therapy is often used alongside other treatments, such as physical therapy or guided exercise.
People sometimes ask how well low-level laser therapy works for chronic pain. While results vary, many notice a gradual improvement as inflammation decreases and healing takes place.
When to Seek Orthopedic Care
Don’t ignore pain that lasts too long. Getting treatment early can prevent injuries from worsening.
Consider seeing an orthopedic specialist if you notice any of the following:
- Joint or muscle pain lasting several weeks
- Injuries that do not improve with rest
- Swelling or stiffness around a joint
- Difficulty returning to normal activities
Seeing a doctor early allows for quicker diagnosis and appropriate treatment recommendations. Additionally, prompt treatment increases the chances that non-surgical options will be effective.
Considering Non-Surgical Options First
Not every orthopedic problem needs surgery. Many injuries improve with treatments that reduce inflammation and support healing.
Treatments such as low-level laser therapy can help relieve pain and improve movement in some conditions. For some people, this may delay surgery or even make it unnecessary.
However, the best treatment always depends on your diagnosis.
If you have joint pain, tendon injuries, or ongoing orthopedic discomfort, the team at Urgent Orthopaedic Care can evaluate your condition and discuss both surgical and non-surgical options. Getting diagnosed early and following the right care plan can help you return to your activities safely and with confidence.
Schedule a consultation with the specialists at Urgent Orthopaedic Care’s Los Angeles or North Hollywood locations to get an accurate diagnosis and explore your treatment options.